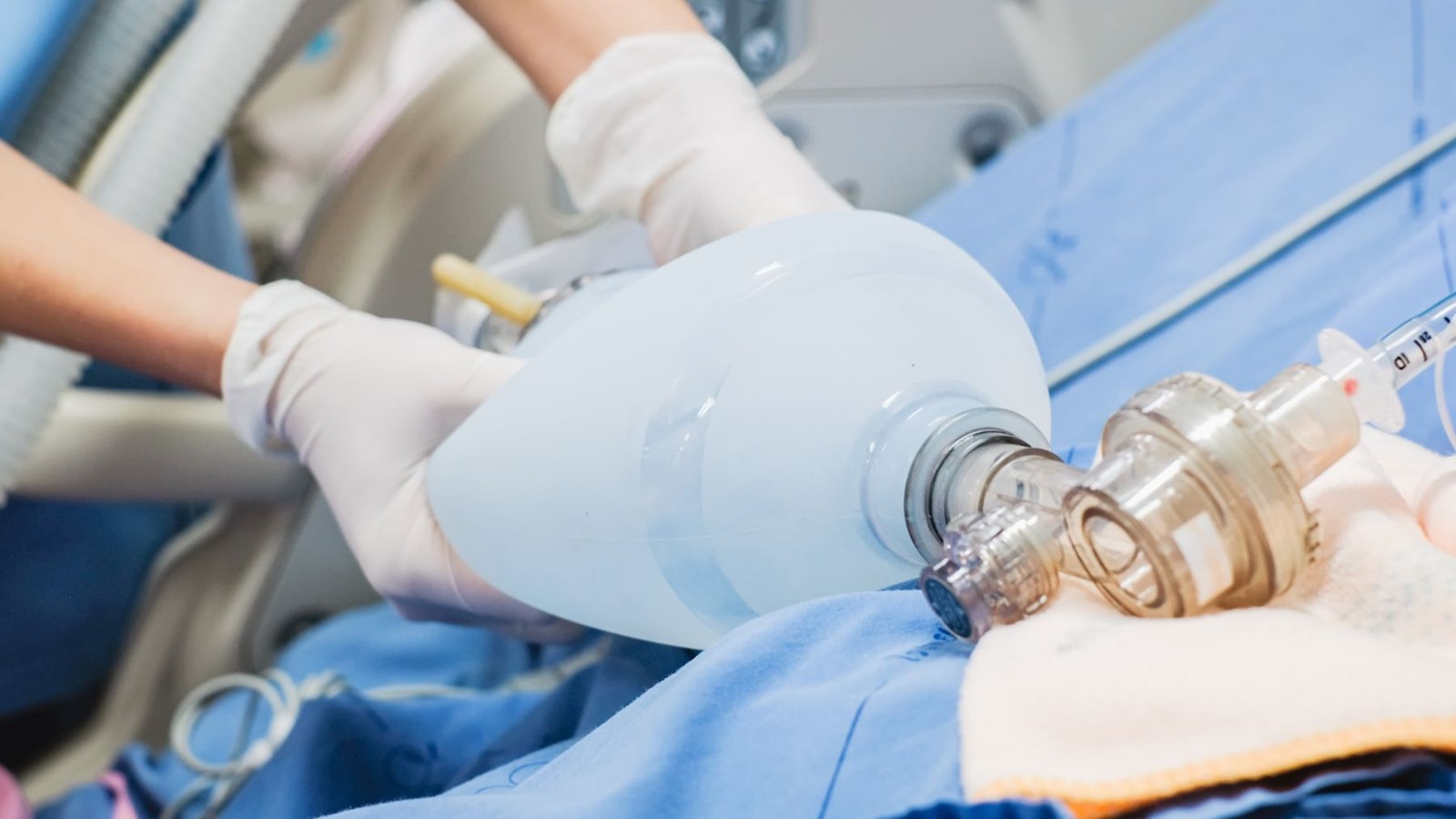
Intensive Care Unit (ICU) dreams are so vivid, that patients very commonly cannot tell the difference between dream and reality. It is often the first thing that they talk about to their relatives on regaining consciousness - with tales of being spied at through the holes in the polysterene-tiled ceiling, a particular doctor or nurse trying to kill them, sexual orgies and babies being born. This, not surprisingly, is likely to be met with a mixture of laughter and anxious concern.
When an ICU patient’s vivid experience is received in this way, they often fear for their sanity - as do their relatives. And a doctor or nurse’s explanation that these are just ‘delusional memories’ may add to their fears.
Vivid dreams and hallucinations in ICU are a common occurrence and one of the major causes of distress for patients who have been in ICU. This particular distress can usually be easily alleviated yet, if not attended to, it can develop into PTSD. I have been contacted by people who had suffered from their recurring ICU nightmares for years.
The rationale for my way of working, experientially developed over a period of almost 20 years, is now supported by recent neuroscientifically-informed trauma therapies: ICU vivid dreams and ICU flashbacks, like other events experienced as traumatic, have bypassed conscious, cognitive processing. They are stored as sensory fragments and, when triggered, these sensory and emotional experiences are then relived in their, usually terrifying, unprocessed form. (And when a dream experience has been traumatic, going to sleep can become a trigger.) When patients can make sense of their vivid dreams, acknowledge and sense their fight for survival, this helps to process and integrate these vivid dreams into a personal, embodied narrative of their ICU journey - a narrative of active survival.
Although each ICU dream tells a different story, ICU vivid dreams and hallucinations usually fall under 10 main themes, of which the most common are: trying to escape and doctors and nurses are trying to kill me, pushing drugs or selling body parts. Patients can be particularly upset and embarrassed about recounting dreams of orgies and babies being born on the unit, which are also very common.
Listening respectfully, providing psychoeducation, normalisation and reassurance are of paramount importance.
In post-ICU dreamwork, the dreamer is helped to move from being caught up in the storyline, imagery and strong emotions of their vivid dreams or hallucinations to articulating it verbally, processing it consciously and gaining a sense of their own powerful attempts to fight for survival. This realisation and ensuing sense of empowerment can be further grounded with bodywork.
From nightmares these dreams can become an empowering testimony to patients’ own resourcefulness. What is more, they can help give some meaning to their ICU experience. Patients may not remember events or medical and nursing interventions that occurred in that ‘lost time’ while they were in ICU, however these dreams and their significance can be integrated within the narrative of their coronavirus journey and, if they wish, the story of their life.
Coronavirus (COVID-19)
Guidance and resources for members

Sharing your experiences
Marking one year since the start of lockdown, we’re sharing your blogs about the impact the coronavirus pandemic has had on you, your practice and your clients

Coronavirus: Advice for the public
Advice on seeing a therapist during the pandemic, plus tips, advice and coping strategies from our members to help you through these uncertain times
Views expressed in this article are the views of the writer and not necessarily the views of BACP. Publication does not imply endorsement of the writer’s views. Reasonable care has been taken to avoid errors but no liability will be accepted for any errors that may occur.