Grief is subjective. It’s unique, individual and can’t be weighed and measured. We’re as different on the inside as we look on the outside. We can never assume how much pain someone is in, and the one thing we should never do in relation to grief and loss is make assumptions.
We do talk about death much more now. But there is still an enormous taboo, because we have a kind of magical thinking that if we talk about death, it might hasten our death or the death of the person we love. This means that when it does happen to people, they’re very ignorant, and it makes what’s already frightening much worse.
The biggest influence of good outcomes following a death is not the circumstances of the death or the personality, it is the recovery environment. The support people are given at the time of, and following, the death will have the greatest influence on the outcome. When love dies, the only thing that helps is the love and support of others. It may be that, as counsellors, we’re part of that network, but on our own, we’re not enough. People see us once or maybe twice a week for 50 minutes. They need a network of support around them to help them survive. We need to recognise the limits of what we influence.
The role of attachment
You will be familiar with Bowlby, and secure and insecure attachment. With loss, what I find helpful is to think of the bereaved person as an oak tree and grief as a storm that comes whistling, cracking through you. For someone who has deep roots, who’s been well watered and has grown in good conditions, you have the capacity to weather the storm. But anyone, who has suffered multiple losses, close to each other, can be shaken to their foundations.
What helps is our capacity to adapt and be flexible, given the circumstances we’re in. If we’re securely attached, we have the capacity to expand and adjust to this new reality that we don’t want. My parents used to talk about forgetting and moving on. I think it is by remembering that you learn to live with the loss. At the beginning, the loss is like a black hole you feel in your stomach. But, as you grieve, although the hole doesn’t necessarily get smaller, you can build your life around it.
When someone comes through your door, what are the signs that this person is likely to be more vulnerable than somebody else? What does this particular death, for this particular individual, at this particular time in their life, living in this community, in these circumstances, mean?
The daughter
Cheryl was a paediatric nurse at a hospital I worked at in London. She found herself shouting at a poor young boy who was very ill and came to see me after this. What unravelled was that her mother had died two years before. It wasn’t a sudden death, so everyone assumed that Cheryl would be fine, as did Cheryl herself; as a result, she didn’t let herself feel any of the pain and told me she felt like a grey capsule. Her mum, who came over with the Windrush generation, modelled for Cheryl a stoic, get-on-with-life, don’t-make-a-fuss attitude. Cheryl didn’t know any other way of dealing with pain. She had a nice husband, a lovely son, and a supportive best friend – but she felt blank and I couldn’t get past the armour she protected herself with.
Often, when someone has died, people don’t want to talk about them because they’re scared, so they tiptoe around. One of the ways I connect with people is to talk about the person who’s died, so I asked Cheryl to bring in things that reminded her of her mum. She brought in a scarf, a brooch and a lovely photograph of her sitting on her mum’s lap. I asked her to describe her mum to me. As she was talking, she picked up her mum’s scarf and smelt it. It smelt of her mum. In that moment, Cheryl’s armour dissolved. Smelling the scarf helped her to allow the memory of her mum to come through her. She sobbed. She realised crying didn’t kill her. Once she could connect with her mum, she could allow herself to look at the guilt she felt about being a nurse and not having been able to fix it when her mum had cancer. She was freed from her numbness, which was worse than the pain.
The sibling
Mussie’s brother, Hashim, shot himself at 21. His presentation to me in counselling as smooth and confident was a protection against fragmentation. He’d been very close to his only brother and felt devastated by his loss. He’d spoken to Hashim the day before he shot himself, and was experiencing the terrible thing that happens with suicide: regret. All the ‘what ifs’: what if I’d noticed? What did I miss? What did I do wrong? Questions that you can never have answers for. Mussie was locked in regrets.
Siblings are often called the hidden mourners and frequently don’t get full acknowledgement of their loss. Mussie’s mother told him, ‘It’s much worse for me. He was in my body. He came out of me.’ So he felt he had to look after his mum. And, as the only remaining son, he felt he had to provide for his father’s future and live up to his unrealistic dreams. Mussie was in real trouble.
You can get completely stuck, going round and round, trying to make sense of suicide. I worked with Mussie using focusing. He had an amazing imagination and found a way of expressing what he felt in his body in images and pictures in his mind, so that what was inchoate in his system became a story that, by talking through, helped him begin to understand himself.
The story spoke for him. By the end of therapy, he was able to make sense of things: Mussie said, ‘We love Hashim, and he will always be alive in us, and we will always love him.’ He’d found a way of living with the reality of his brother’s death and allowed himself to still love him.
The parents
I work with a couple whose child died and the male partner lost his job. The relationship was in trouble because they were both grieving very differently. They had no hope. They tried to get pregnant. She tried three rounds of IVF. It didn’t work. The work we did was accepting that they didn’t at this point have hope. I couldn’t infuse hope in them because life had been so devastating for them. I worked with what not having hope meant for them. A big part of loss is the change in your identity. Am I still a parent, if I have a child who dies? Am I still a partner, if I’m not getting on with my partner? Am I still a useful person, if I lose my job? They needed good things to happen, which eventually did. He got a job and they did have a child, but it took a long time.
The paradox of pain
My basis for believing there is a ‘paradox of grief’ is taken from Rogers’ ‘paradox of change’: that the more you accept the aspects of yourself that you find unacceptable, the more likely it is that change will occur. When we’re grieving, the paradox is that we’re forced to face a reality we don’t want to face, which we don’t want to be true. Everything in our system wants to block the fact that it’s true, but it’s an impenetrable wall. We can’t get past it.
In the 21st century, when everything is so fast, people find the endurance, pain and powerlessness of grief particularly difficult. The very thing that allows us to face the reality of the loss is the thing that no-one wants: pain is the agent of change. Pain is the thing that forces us to know the reality: that our partner who was sitting beside us, or our mother, or our child, or our sibling, or our friend, is now irrevocably, irreversibly dead.
I hate terms like ‘loss’ or ‘gone to a better place’; I find them infuriating. I always use the word ‘dead’. From my experiences with clients, it’s the thing that people do to avoid the pain that does them harm: ‘If I let myself feel this pain, I’m never going to survive.’ It’s a paradox because the truth is that, if they allow themselves to feel the pain, incrementally, for a moment, it forces their system to adjust to this new reality. Pain is what heals you.
But people think, ‘If I hold on to the pain, I hold on to the person. If I let go of the pain, I’m abandoning and leaving the person I love.’ The work is to allow both: to know that you can hold on to the pain, and actually you need to hold on to the person, but only when you’ve faced the reality that they’ve died. Death may steal a future, imagined and assumed, but it doesn’t steal the relationship. The love doesn’t die. That’s key. The thing that takes a lot of time in sessions is that pitch battle between the head and the heart because they do not speak the same language.
There is often a conflict between the head and the heart. The person knows, logically, they are not guilty, but in their heart, they feel they are. The work is to allow both parts of the person to speak, and have an equal voice for both their head and their heart, not trying to knock each other out in a pitched battle.
Dual process: loss and restoration
I’m very grateful to Elisabeth Kübler-Ross, but sick to death of people talking about stages of grief. She was an amazing woman, she did great work, and she never expected grief to be this machine that you’re meant to go through: that you start on the ground floor of denial and then you get to the top of acceptance. Stroebe and Schut1 realised from their research that we need a dual process. We need to experience, express and allow the loss. We have loss orientation and this oscillates with restoration, with this idea of hope, of having a future, of moving on and having a break from the pain. Allowing ourselves to do both is how we heal. At the beginning, people are very loss oriented, but, over time, if they get the right support, it frees them to have a break from the pain, to go back to work, go for a run, see a friend. That gives them the psychological energy to come back and do some of the loss work. They move between the two.
The work is in the movement. Women tend to be loss oriented. They tend to ruminate, and research shows this.1 Men tend to be restoration oriented: they want to get on. They want to have another child. They want to go back to work. When I’m with couples, I tell them about this research and notice the relief on their faces when they see he isn’t a selfish bastard, she isn’t a complete wet rag, but actually they’re just being their evolutionary selves, and can support each other: she can help him do some of the loss work and he can help her have some hope and do some of the restoration work. Children of both genders naturally do both. What we talk about in Child Bereavement UK is that it’s like jumping in and out of puddles. A child can be very sad, crying, and you think, ‘Oh my God, when are they ever going to stop?’ Then, suddenly, they’re laughing and playing, and they’re fine.
As adults, because we want to stop them screaming, we say, ‘Don’t cry. It’s OK. You don’t need to be sad; you’re going to be all right.’ What we need to do is to let them feel sad, let them do what they need to do and be normal kids; so they do this oscillation of moving in and out of grief very naturally.
How we heal in grief is by both allowing ourselves to feel pain, but also finding a way of building the relationship with the person who’s died in our life, so that they are always a part of us. This may be by wearing their watch, by thinking of them in heaven, by having a bench in the garden where we go and remember them. People who have lost someone often talk to the person who’s died: ‘Dad, should I marry this guy?’ ‘Do you mind if I have another lover?’ ‘Will you forgive me?’ People maintain a relationship with them (but may feel they’re bonkers doing so). We need to encourage them to recognise that it’s healthy and normal to have this relationship, as long as you have faced the reality that they’re actually dead. It’s immensely healing having the relationship. It becomes part of you. Having hope is a way of learning to live with the loss. Doing things that help us to connect with the person who’s died, integrates the mind and body in a very helpful way.
Finding structure
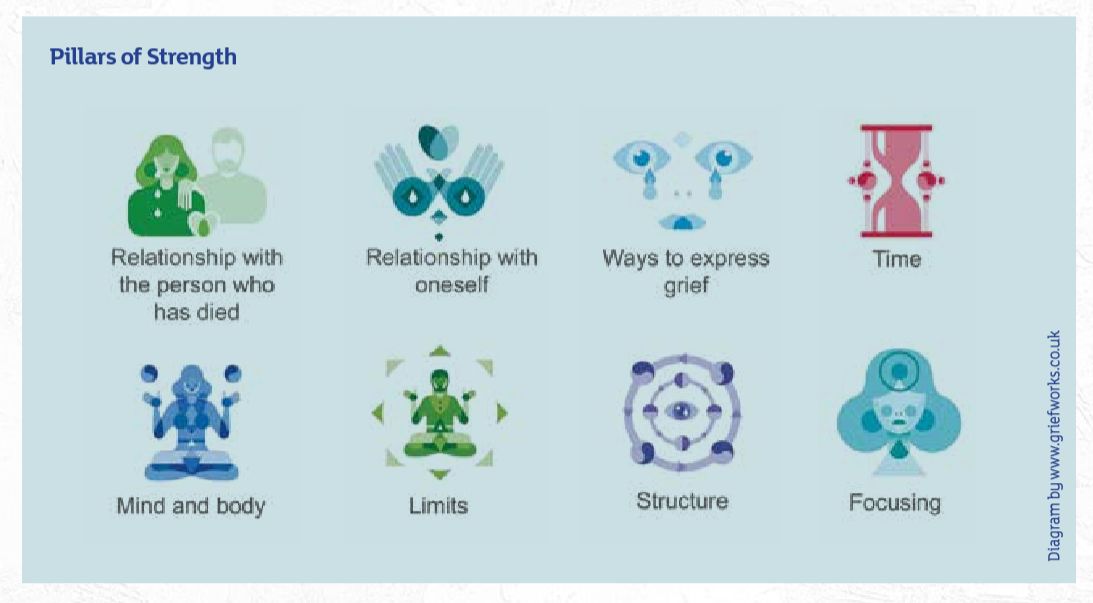
I have developed the idea of ‘pillars of strength’ (see diagram) as the key structures that support us and enable us to rebuild our life. It requires work to build the pillars – they don’t just appear out of the blue – and commitment to keep going; they work as an integrated whole. We can’t just focus on one pillar, they all require our attention and time. And there is a multiplier effect working on all the pillars, which increases their strength.
It came about because people have this black hole in them. I thought that, if you give them structures, pillars that they can hold on to when they feel they have nothing to hold on to, it can allow them to weather the storm. The relationship with oneself is key. One of the terrible cruelties of grief is that people attack themselves. They feel like they’re failing. They blame themselves and are nastier than they ever would be to anybody else. One of the things I advise is to treat yourself as if you were talking to your best friend. Have self-compassion and try and be kind to yourself.
Grief is a small word that describes a vast, messy and chaotic process, which feels like it takes you over. You feel like the world is ruling you and you have no power. Developing attitudes of being kind to oneself, connecting with the person who has died, and developing good habits, supports you to build firm foundations when you feel you are crumbling.
Julia Samuel MBE, Msc, MBACP (Snr Accred), UKCP was psychotherapist for paediatrics at St Mary’s Hospital Paddington, the post she established in 1992. Her role for 25 years involved seeing families who have children or babies who have died, and training and supporting staff. In 1994, she helped launch and establish the Child Bereavement Charity, and, as the Founder Patron, was involved and continues to be involved in many aspects of the charity’s work, having a key role in fundraising, strategy and training. In 2016, Julia was awarded an MBE in recognition of her services to bereaved children, and in 2017 Middlesex University awarded her an Honorary Doctorate. In 2017, Julia published Grief Works: stories of life, death and surviving (Penguin Life), which was a bestseller in the UK and has been published in 16 countries. She also has a private practice where she sees families and individuals for many different issues. griefworks.co.uk
Reference
1. Stroebe MS, Schut H. The dual process model of coping with bereavement: rationals and description. Death Studies 1994; 3: 197–224.